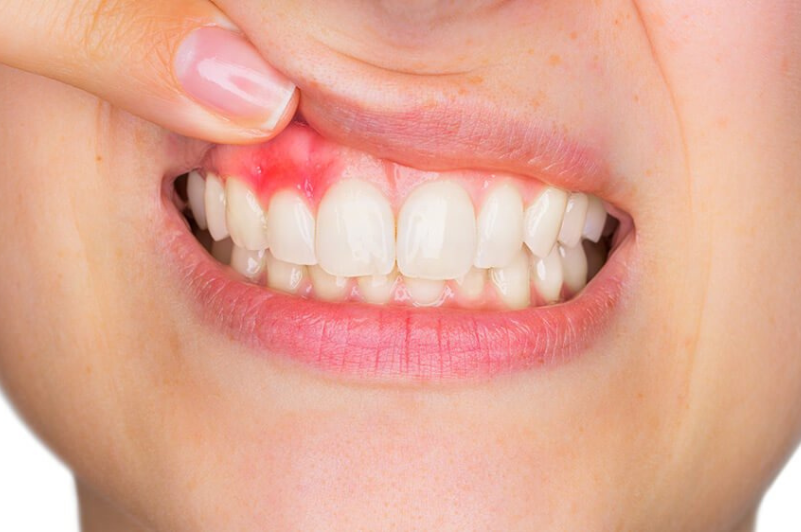
Bad breath — medically known as halitosis — is one of the most common yet underestimated dental concerns. For many people in Dallas, it’s easy to reach for a breath mint and move on. But when bad breath becomes persistent, it can be a sign of something more serious lurking beneath the gum line: a gum infection.
Understanding the link between bad breath and gum disease is the first step toward protecting your oral health — and your overall well-being. This guide breaks down the causes, symptoms, and available treatments, so you know exactly what to watch for and when it’s time to see a dentist.
Important: Gum disease is often painless in its early stages. Don’t wait for discomfort to seek care. Catching it early makes treatment faster, easier, and far more effective.
What Is a Gum Infection?
A gum infection — commonly referred to as gum disease or periodontal disease — occurs when bacteria build up along and beneath the gum line, causing inflammation, tissue damage, and in advanced cases, bone loss. It begins with a mild condition called gingivitis and can progress to a more severe form known as periodontitis.
The bacteria responsible for gum infections thrive in the warm, moist environment of your mouth, particularly when oral hygiene habits slip. As they multiply, they release toxins that irritate gum tissue and produce foul-smelling gases — the primary reason why gum infections and bad breath so often go hand in hand.
The Three Stages of Gum Disease
Gingivitis
The earliest and most reversible stage. Gums become red, swollen, and may bleed when brushing. There is no bone or tissue loss yet. Good oral hygiene and a professional cleaning can often fully reverse it.
Periodontitis
The infection has spread below the gum line, causing pockets to form between the teeth and gums. Bone and tissue damage begins to occur. Professional treatment is required to halt progression.
Advanced Periodontitis
Pockets deepen significantly and may fill with pus. Teeth become loose and extremely sensitive. In severe cases, tooth removal may be necessary to prevent the infection from spreading further.
Common Causes of Bad Breath and Gum Infections
Bad breath linked to gum infections doesn’t arise overnight — it develops as a result of several contributing factors. Understanding these causes can help you take meaningful preventive action.
🦠Plaque & Tartar Buildup
When plaque isn’t removed through regular brushing and flossing, it hardens into tartar. This creates a breeding ground for bacteria that releases odor-causing compounds.
🚬 Smoking & Tobacco Use
Tobacco use weakens the immune system’s ability to fight gum infections, reduces saliva flow, and dramatically worsens bad breath.
💧Dry Mouth (Xerostomia)
Saliva naturally washes away bacteria and food particles. Without enough of it, bacteria multiply quickly, leading to both gum disease and bad breath.
⚕️Missed Dental Visits
Skipping routine dental exams and cleanings allows plaque and early gum disease to go undetected and untreated.
🍬Poor Diet
Diets high in sugar and processed foods fuel bacterial growth in the mouth, increasing the risk of both cavities and gum infections.
🧬Medical Conditions
Diabetes, hormonal changes, and certain medications can all compromise gum health and contribute to chronic bad breath.
Signs of a Gum Infection Linked to Bad Breath
- Persistent bad breaththat doesn’t improve with brushing, flossing, or mouthwash
- Red, swollen, or tender gumsthat look inflamed or feel sore to the touch
- Bleeding gumsduring or after brushing and flossing
- Receding gumsthat make your teeth appear longer than normal
- Loose or shifting teethas bone and tissue support weakens
- Pus or dischargebetween the teeth and gums
- Pain when chewingor sensitivity along the gum line
- A metallic or unpleasant tastein the mouth that lingers
If you notice any combination of these symptoms, it’s time to act. Early intervention can prevent minor gum irritation from becoming a serious infection.
Schedule a dental appointment in Dallas as soon as possible.
Treatment Options for Gum Infections and Bad Breath
The good news is that gum disease — even in its more advanced stages — is treatable. The right approach depends on the severity of the infection, and your dentist will tailor a plan specifically for your situation.
Non-Surgical Treatments
1 Professional Dental Cleaning
For gingivitis and mild gum disease, a thorough professional cleaning removes plaque and tartar buildup that brushing at home simply cannot reach. This is often all that’s needed in the earliest stage.
2 Scaling and Root Planing (Deep Cleaning)
For moderate to advanced cases, scaling removes bacteria and tartar both above and below the gum line, while root planing smooths the tooth root surfaces to help gums reattach and heal properly. This non-surgical “deep cleaning” is the most common first-line treatment for periodontitis.
3 Antibiotic Therapy
Your dentist may prescribe topical or oral antibiotics to target bacteria in the gum pockets and help control the infection alongside mechanical cleaning.
Surgical Treatments
Addressing an Underlying Infection
Sometimes bad breath and gum discomfort are tied not just to gum disease, but also to a deep tooth infection. When bacteria reach the inner pulp of a tooth, it can cause an abscess — which produces a notoriously foul odor. In these cases, root canal therapy is often the most effective solution to eliminate the infection and preserve the natural tooth.
How to Prevent Bad Breath and Gum Infections
Prevention is always the best strategy when it comes to gum health. A consistent oral hygiene routine, combined with regular professional care, can keep gum disease from developing in the first place.
Brush twice dailyusing a soft-bristled toothbrush and fluoride toothpaste, spending at least two minutes each sessionFloss at least once a dayto remove plaque and debris from between teeth where your toothbrush can’t reach Use an antibacterial mouthwashto reduce bacterial load in hard-to-reach areas of the mouth Stay hydratedthroughout the day to maintain healthy saliva flow and wash away food particles Avoid smoking and tobacco products, which dramatically increase your risk of gum disease and chronic bad breath Eat a balanced dietlow in sugar, with plenty of vegetables, lean proteins, and calcium-rich foods
Visit your dentist every six monthsfor a professional general dentistry check-up and cleaning
When Should You See a Dentist in Dallas?
You should seek professional dental care promptly if you notice:
- Bad breath that persists for more than a few days despite good oral hygiene
- Gums that bleed regularly when you brush or floss
- Any visible swelling, pus, or a “pimple-like” bump on your gums
- Teeth that feel loose or have shifted in position
- Sudden or increasing pain when biting or chewing
At DentUrgent in Dallas, our team offers same-day appointments and extended hours on weekdays and weekends, so you never have to wait when a dental concern arises. Early treatment protects your smile and prevents a manageable problem from becoming a major one.
Frequently Asked Questions on Root Canal Treatment
Can bad breath be a sign of a serious gum infection?
Yes. While bad breath can have many causes — including diet and dehydration — persistent halitosis is one of the most common early symptoms of gum disease. The bacteria responsible for gum infections release volatile sulfur compounds, which produce a strong, unpleasant odor. If your bad breath doesn’t improve with brushing and flossing, a dental evaluation is important.
How do I know if I have gingivitis or a more advanced gum infection?
Gingivitis typically presents as red, puffy gums that bleed during brushing, without pain or significant tissue loss. More advanced periodontitis involves deeper gum pockets, receding gum lines, loose teeth, and possible pus between the gums and teeth. A dentist can accurately diagnose your stage with a periodontal exam and X-rays.
Is gum disease reversible?
Gingivitis — the earliest stage — is fully reversible with professional cleaning and improved home care. Once gum disease advances to periodontitis, the bone and tissue damage that has already occurred cannot be completely undone, but the condition can be effectively managed and halted with proper treatment to prevent further damage.
What happens if a gum infection is left untreated?
Untreated gum infections can progress to advanced periodontitis, leading to significant bone loss, loose teeth, and eventual tooth loss. Beyond your mouth, research links untreated gum disease to systemic health issues, including increased risk of heart disease, diabetes complications, and respiratory problems.
Can gum disease be treated without surgery?
In many cases, yes. Mild to moderate gum disease is effectively treated with professional deep cleaning (scaling and root planing) combined with good at-home oral hygiene. Surgery is generally only considered when the disease has progressed to a point where non-surgical methods cannot adequately clean the infected areas or restore tissue health.
How often should I visit the dentist to prevent gum disease?
Most dental professionals recommend visiting every six months for a routine exam and cleaning. However, patients with a history of gum disease or other risk factors may benefit from more frequent visits — typically every three to four months — to keep the condition under control.
Can a tooth infection cause bad breath?
Absolutely. A dental abscess — an infection inside the tooth pulp — produces a distinct and often severe bad odor. If you suspect a tooth infection alongside bad breath and gum pain, you may need root canal treatment to remove the infected tissue and eliminate the source of the odor.